What is Colorectal Cancer?
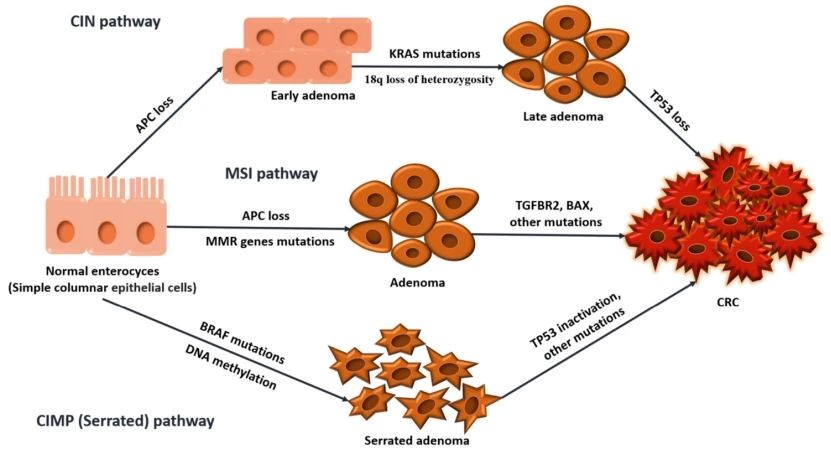
Colorectal cancer is a common malignant tumor in the gastrointestinal tract, with incidence second only to gastric and esophageal cancers. It constitutes the most frequent type of large intestine cancer (accounting for about 60%) and is mainly divided into two categories: colon cancer and rectal cancer. The majority of patients are over 40 years old, with approximately 15% under 30. It is more common in males, with a male-to-female ratio of 2-3:1. Clinical observations indicate that the occurrence of colorectal cancer is closely associated with high-fat, low-fiber diets, genetic factors (e.g., Lynch syndrome), chronic intestinal inflammation (e.g., ulcerative colitis), as well as obesity and lack of exercise.
In Indonesia, colorectal cancer ranks as the sixth most common cancer for both men and women. According to 2022 data, Indonesia reported approximately 18,300 new colorectal cancer cases annually (10,500 males and 7,800 females), placing it among the leading causes of cancer-related deaths. Due to low early screening rates, about 65% of patients are diagnosed at intermediate or advanced stages, resulting in a 5-year survival rate of only 35%-40%, presenting a severe challenge for prevention and treatment.
What are the diagnostic methods for Colorectal Cancer?
1. Fecal Occult Blood Test (FOBT)
A preliminary test for individuals without noticeable colorectal cancer symptoms. It detects microscopic blood in small stool samples that is invisible to the naked eye, indicating potential intestinal bleeding.
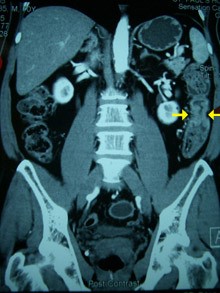
1. CT Colonography
A non-invasive follow-up examination. Uses computed tomography to capture two- and three-dimensional images of the intestines. If abnormalities are found, a colonoscopy is required for further investigation (see example image below).
2. Colonoscopy
Recommended for individuals with abnormal preliminary test results or those at higher risk of colorectal cancer. This method involves inserting a flexible tube with a small camera through the anus into the rectum, passing through the sigmoid colon, descending colon, transverse colon, ascending colon, and reaching the cecum for examination. Polyps can be removed and tissue samples collected for biopsy during the procedure.
3. Sigmoidoscopy
Similar to colonoscopy but examines only the rectal lining and the lower half of the colon (covering ~50% of the total rectal/colon area). Carries relatively lower medical risks compared to full colonoscopy.
What treatment options are suitable for different stages of Colorectal Cancer?
1. Carcinoma in situ
Endoscopic treatment is effective and can achieve complete cure.
2. Early-stage colorectal cancer
Surgical resection can achieve complete cure. Some cases may also be treated endoscopically with curative intent.
3. Locally advanced colorectal cancer
Comprehensive treatment with surgery as the main approach, supplemented by adjuvant chemotherapy, targeted therapy, and radiotherapy post-operation.
4. Inoperable locally advanced colorectal cancer
Radiotherapy, chemotherapy or targeted therapy may be selected based on disease condition to improve patient survival.
5. Recurrent or metastatic colorectal cancer
Chemotherapy or targeted therapy can be used. Selected patients may undergo surgery to prolong survival.
6. Recurrent or metastatic rectal cancer
Treatment primarily consists of chemoradiotherapy or targeted therapy, with surgery generally not indicated.
What are the treatment options for colorectal cancer?
Surgical Treatment
• Curative surgery: Suitable for early-stage colorectal cancer. For example, right-sided colon cancer may be treated with right hemicolectomy. Early-stage rectal cancer with small tumor size, limited to the mucosa or submucosa, and high differentiation may undergo local excision. Rectal cancer located more than 5 cm above the dentate line may be treated with anterior resection (Dixon surgery), while rectal cancer below the peritoneal reflection often requires abdominoperineal resection (Miles surgery).
• Palliative surgery: Suitable for advanced cases with distant metastasis but where the local tumor is still resectable. Depending on the patient's overall condition and local disease extent, options include palliative resection, bypass surgery, or colostomy to relieve symptoms and prolong survival.
Chemotherapy
• Neoadjuvant chemotherapy: Uses chemical drugs to shrink tumors, downstage the disease, improve surgical resection rates, and eliminate potential micrometastases.
• Adjuvant chemotherapy: Targets residual cancer cells after surgery to reduce recurrence risk and extend survival.
• Palliative chemotherapy: For advanced, unresectable, recurrent, or metastatic colorectal cancer, it controls tumor growth, alleviates symptoms, and prolongs survival.
Radiotherapy
• Neoadjuvant radiotherapy: Reduces tumor size and adhesion to surrounding tissues, improving surgical success rates and lowering local recurrence risk.
• Adjuvant radiotherapy: For high-risk patients with positive surgical margins or lymph node metastasis, it further eliminates residual cancer cells.
• Palliative radiotherapy: Relieves symptoms such as pain and bleeding in advanced cases, improving quality of life.
Targeted Therapy
By identifying and blocking specific cancer-related proteins (e.g., EGFR mutations), it restricts tumor cell proliferation and disrupts growth signaling pathways. It is suitable for metastatic colon cancer patients with specific genetic mutations.
Immunotherapy
Enhances the body’s antitumor immunity, such as through PD-1/PD-L1 inhibitor monoclonal antibodies, restoring T cells' ability to recognize and attack cancer cells expressing specific proteins. It is suitable for colorectal cancer with microsatellite instability-high (MSI-H) or mismatch repair deficiency (dMMR).
Interventional Therapy
• Arterial infusion chemotherapy: Delivers high-dose drugs directly to tumor-feeding arteries for precise cancer cell elimination.
• Cryoablation: Uses extreme cold to "freeze" tumors, particularly effective for liver metastases.
• Radiofrequency ablation: Aims to "burn" metastatic cancer cells.
• Radioactive Iodine Seed Implantation: Involves embedding radioactive particles directly into the tumor to continuously destroy cancer cells.

